Multiple sclerosis or MS is a chronic disease affecting the brain and spinal cord (central nervous system). Nearly 3 million worldwide are living with MS.
It is the most common acquired chronic neurological disease affecting young adults. Diagnosis often occurs between the ages of 20 to 40. In Australia, it affects three times more women than men.
As yet, there is no cure for multiple sclerosis, but there are treatments available to manage symptoms and help individuals recover faster from attacks.
What causes multiple sclerosis?
There is no known single cause of MS. Studies have shown that many genetic and environmental factors contribute to its development. For example, you’re more likely to develop MS if you have a close relative with MS or another autoimmune disease.
In MS, the immune system attacks the protective sheath called myelin that covers nerve fibres. Myelin protects the nerve fibres and helps them send signals from the brain to the rest of the body quickly and efficiently.
Damage to the myelin causes communication problems between the brain and the rest of the body. It can also eventually cause permanent damage of the nerve fibers as they become exposed and scarred.
What are the symptoms of multiple sclerosis?
Symptoms vary widely from person to person and can also come and go. It depends on the location of the nerve damage and how much damage has occurred.
Common symptoms include:
- Vision problems, eg blurred or double vision, blind spots or pain during eye movement
- Unusual sensations, such as pins and needles, tingling or electric-shock sensations
- Changes in memory, concentration or thinking
- Trouble with walking
- Numbness or weakness
- Depression and anxiety
- Slurred speech
- Vertigo
- Fatigue
How is multiple sclerosis diagnosed?
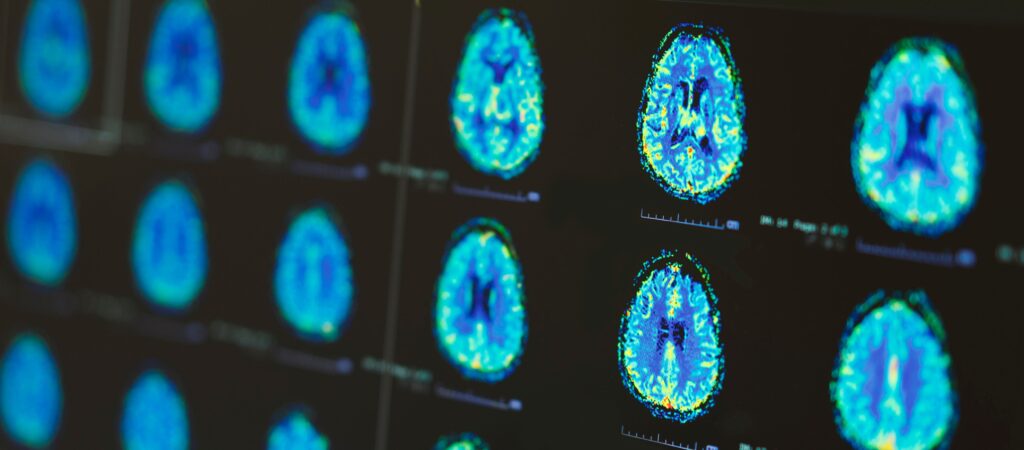
Diagnosis requires a combination of tests and check-up with a neurologist. An imaging procedure called magnetic resonance imaging or MRI will be conducted to detect areas of damage in the brain and spinal cord. Other tests may be carried out to test nerve activity.
Relapsing-remitting MS (RRMS) is the most common form of MS. People with RRMS experience periods of new symptoms or relapses that develop over days or weeks. These symptoms then usually improve partially or completely, followed by quiet periods of disease remission that can last months or even years.
Secondary-progressive MS (SPMS) eventually develops in at least 20 to 40% of those with RRMS. This is characterized by a steady progression of symptoms, with or without periods of remission, within 10 to 20 years from the start of the disease.
Primary progressive MS (PPMS) is diagnosed in about 1 in every 10 people with MS. In this type, symptoms become gradually worse from the start of the illness, with no separate attacks or periods of remission.
Treatments and management
According to MS Australia, 64% of people with MS use a disease modifying therapy (DMT) or immunotherapy.
These are medicines that target the immune system, making relapses less frequent and severe.
For people with RRMS, DMTs can slow down or prevent their disease from developing into secondary-progressive MS.
Other medicines are available to ease specific MS symptoms. For example, you may undergo physiotherapy for muscle problems, or access counselling and medication to manage mood problems.
Decisions about any treatments should be made in careful consultation with your neurologist and healthcare team.
Supports and services for multiple sclerosis

At Afea, we provide support to people with complex diagnoses, including people living with MS.
As MS symptoms are diverse, participants require different levels of care and assistance.
With our Afea Carers, clients are ensured a clean and safe environment at home, participation in community life and companionship and emotional support during challenging moments.
Contact us now and we’ll develop a care plan designed just for you.